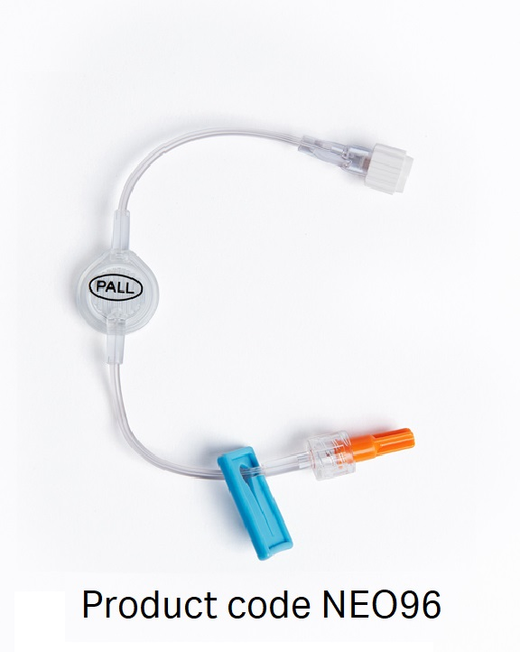
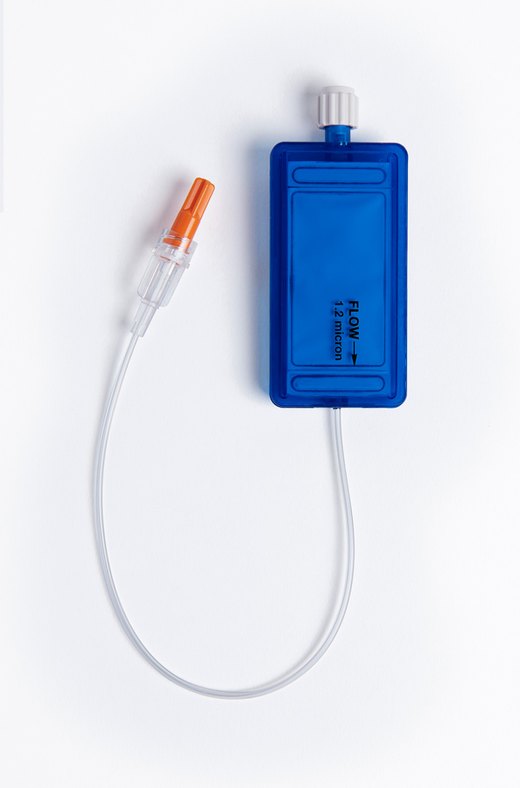
Clinical benefits of in-line IV filters
SUMMARY
Multiple clinical and in-vivo studies have highlighted the potential benefits of in-line IV filters for the most critically ill patients. In-vivo studies have shown that particles compromise microvascular circulation and in-line IV filters can prevent further loss of capillary density in vital organs. Clinical studies have shown that in-line IV filters may preserve organ function and reduce inflammation supporting improved outcomes for ICU patients.
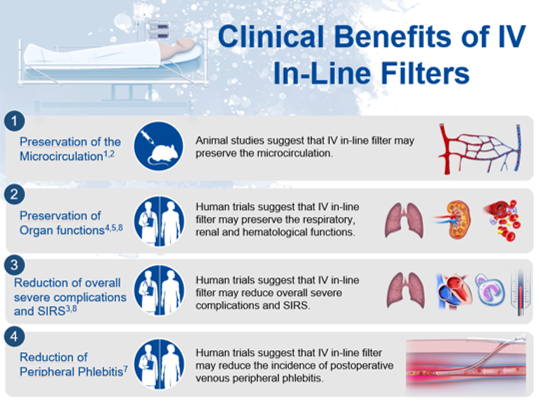
What clinical benefits do IV in-line filters provide?
The impact of particles or the impact of IV in-line filters retaining particles on ICU patients has been in the spotlight of researchers and clinicians since 2008. Pall Medical IV filter has been and continues to be a driving force in this regard.
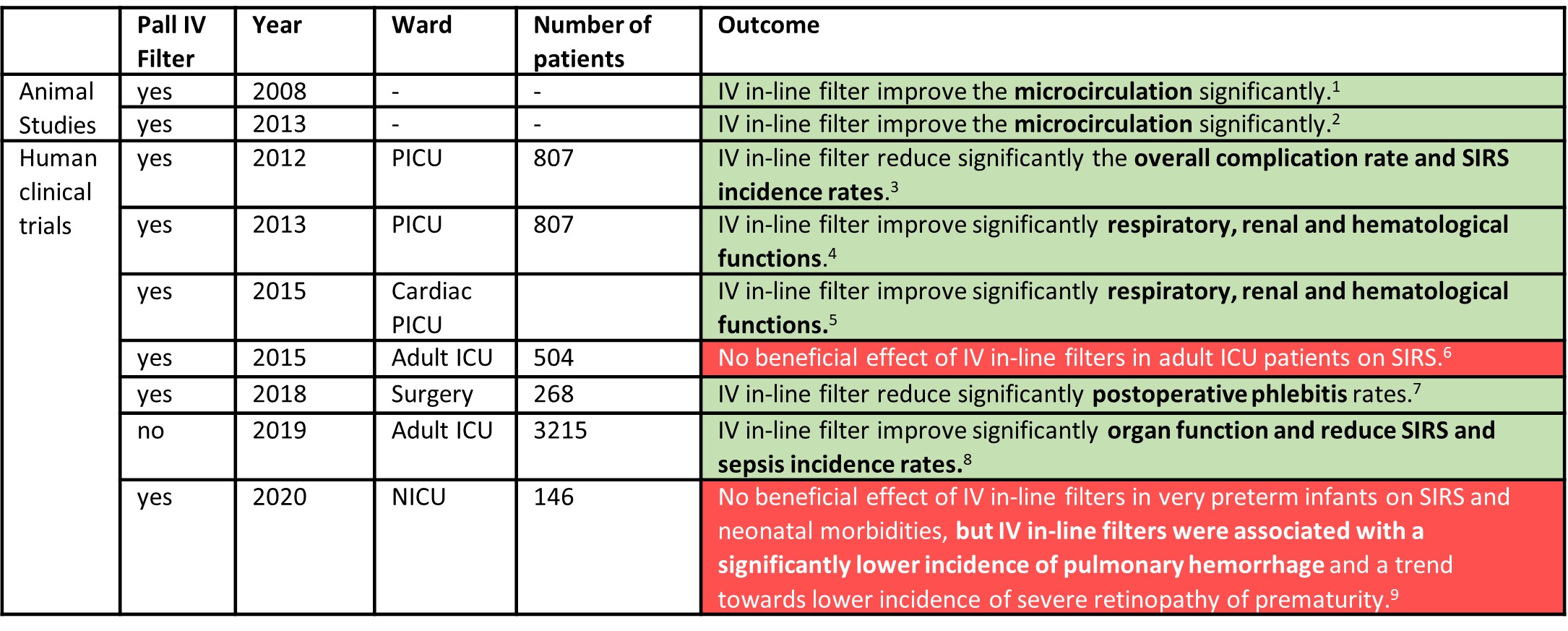
Several animal studies and human clinical trials have demonstrated the clinical benefits of using Pall IV in-line filters.
Animal models demonstrate that infusion of particles pose a major threat to critical tissue perfusion and that IV in-line filters prevent further reduction of postischemic functional capillary density. The results of the animal studies suggest that “in-line filters have potentially enormous relevance for patients with prior microvascular compromise of vital organs (i. e. post trauma, major surgery, sepsis).”1,2
Human clinical trials suggest that IV in-line filters have a positive impact on ICU patients by preserving organ functions and reducing inflammation rates.3-9
Explore our IV particle retention solutions
References
1.Melchore JA. (2011). Sound practices for consistent human visual inspection. AAPS Pharm Sci Tech;12 (1): 215-221
2.Perez M. et al. (2017). Dynamic Image Analysis To Evaluate Subvisible Particles During Continuous Drug Infusion In a Neonatal Intensive Care Unit. Scientific Reports; 7 (9404): 1-8
3.Perez M. et al. (2018). Effectiveness of in-Line Filters to Completely Remove Particulate Contamination During a Pediatric Multidrug Infusion Protocol. Sci Rep; 8 (7714): 1-8
4.Keck C.M., Ngyen M., Pyo S. et al. (2016). How Many Nanoparticles Enter A Patient During Infusion Therapy? The Journal of Vascular Access; 17 (4): e8
5.Benlabed M. et al (2018). Analysis of particulate exposure during continuous drug infusion in critically ill adult patients: a preliminary proof-of concept in vitro study. Intensive Care Medicine Experimental; 6 (38): 1-9
6.Ernst C, Keller M., Eckstein J. (2012). Micro-Infusion Filters and Particulate Matter in Injections. Pharm. Ind; 74 (12): 2009-2020 (German Language)
7.Puntis J.W., Wilkins K.M., Ball P.A., Rushton D.I., Booth I.W. (1992). Hazards of parenteral treatment: do particles count?. Arch Dis Child;67 (12):1475-1477
8.Oie S, Kamiya A. (2005). Particulate and microbial contamination in in-use admixed parenteral nutrition solutions. Biol Pharm Bull; 28 (12): 2268-2270.
9.Ga Eul Joo, Kyeong‑Yae Sohng, Michael Yong Park. (2016). The effect of different methods of intravenous injection on glass particle contamination from ampules. SpringerPlus; 5 (15): 1-8
10.Perez M. et al. (2018). Effectiveness of in-Line Filters to Completely Remove Particulate Contamination During a Pediatric Multidrug Infusion Protocol. Sci Rep; 8 (7714): 1-8
11.Ernst C, Keller M., Eckstein J. (2012). Micro-Infusion Filters and Particulate Matter in Injections. Pharm. Ind; 74 (12): 2009-2020
Author bio
Dr. Volker Luibl, MBA
Dr. Luibl is a Sr. Marketing Manager Medical Content with knowledge in medical device and clinical science.
Need expert help with medical filtration? We can assist you!
*Products displayed on this website may not hold regulatory approval, authorisation, or clearance in all countries, and their availability is subject to regional regulatory requirements. For local office contact information, visit our contact page